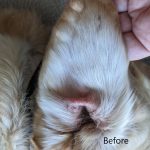
Ear hematoma in dog is an affliction which gets too much attention for needing surgery to repair. In fact, surgery seems to cause more damage than the hematoma itself. First, let’s look at the cause. Something has happened to rupture a feeding artery into the pinna. An underlying condition contributing to ear irritation most likely made the dog rake the ear against something or shaking the ear repeatedly. Either way, an artery is the only blood vessel strong enough to release fluid pressure to tear apart the tissues binding the skin and cartilage. These tears as well begin releasing fluids into the now ever-growing hematoma being created. Here is where different approaches to treatment occur. Should the vet address the blood pool only and aspirate once or multiple times? Should the vet incise the ear and suture the skin back to the cartilage? Should the vet install a drain or allow fluids from the bleeding vessels to exit the ear? In my opinion Yes, No and No. Aspiration alone relieves fluid buildup without harming or wounding. If coagulation has already begun, then a hypodermic needle aspiration will be non-effective. With an early onset hematoma, a hypodermic needle aspiration is pet and pet parent friendly with both relieving the pain for the animal and keeping costs down for owner. However, aspiration is not going to fix the broken blood vessel. The only way to repair the broken blood vessel feeding the hematoma is to allow the animal time to build reparative tissues to seal the break. These repairs take place while the aural hematoma condition is in suspension, meaning the hematoma is no longer filling, the fluids become still allowing for rapid coagulation to begin growing granulation against both skin and cartilage, and the once flowing broken blood vessel now has back pressure against it and the site of break begins to seal and heal. This occurs naturally in untreated aural hematoma. Consequences are that the bulbous blood clot formed is reduced in a fashion where granulation has attached all skin and cartilage to the blood clot, and as the clot is reduced towards the center, the skin and cartilage are pulled along with it causing the shrivel. Since in this scenario the amount of shrivel is proportionate to the diameter of the blood clot, then the solution would be to limit the blood clot size to as thin a layer as possible, making the skin and cartilage in as close proximity as possible at time of blood clot coagulation and granulation. This process is not foreign to veterinary medical. Splinting the auricle for a duration of time will achieve natural healing by allowing a thin layer of blood clot to form in the entirety of the hematoma region. The thin layer acts in the same fashion as a natural bulbous clot, but without the consequences of crinkling the ear after reabsorption. Keeping an open mind to aural splinting for aural hematoma can and will bring new Holistic medical treatments needed to address the current clinical duress patients and their owners are now having to endure.
Ear hematoma in dog is an affliction which gets too much attention for needing surgery to …
Browse Topics: